03/08/20
How schistosome worms defy host immune systems

By: Claudia Caruana
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[NEW YORK] Researchers uncovered in a new study how schistosomes, parasitic flatworms that infect more than 200 million people in the tropics, trick the host’s immune system and continue producing eggs for decades.
Schistosomiasis, caused by schistosome infection, is a neglected tropical disease that is spread by contact with infected snails, according to WHO. Children are particularly vulnerable to schistosomiasis — also known as bilharzia — which causes anaemia, stunting and learning disorders.
Jayhun Lee and his colleagues at the Morgridge Institute for Research, University of Wisconsin–Madison, explain in a report in PNAS how a specialised gland in the parasite’s digestive tract, called oesophageal gland, is behind an immune-evasion mechanism essential for its survival while in its host.
Lee says one feature of schistosomes — which have a complex life cycle which begins in freshwater contaminated with human excrement — is that the mature parasites can live for a decade or more inside the host’s bloodstream where immunity is active.
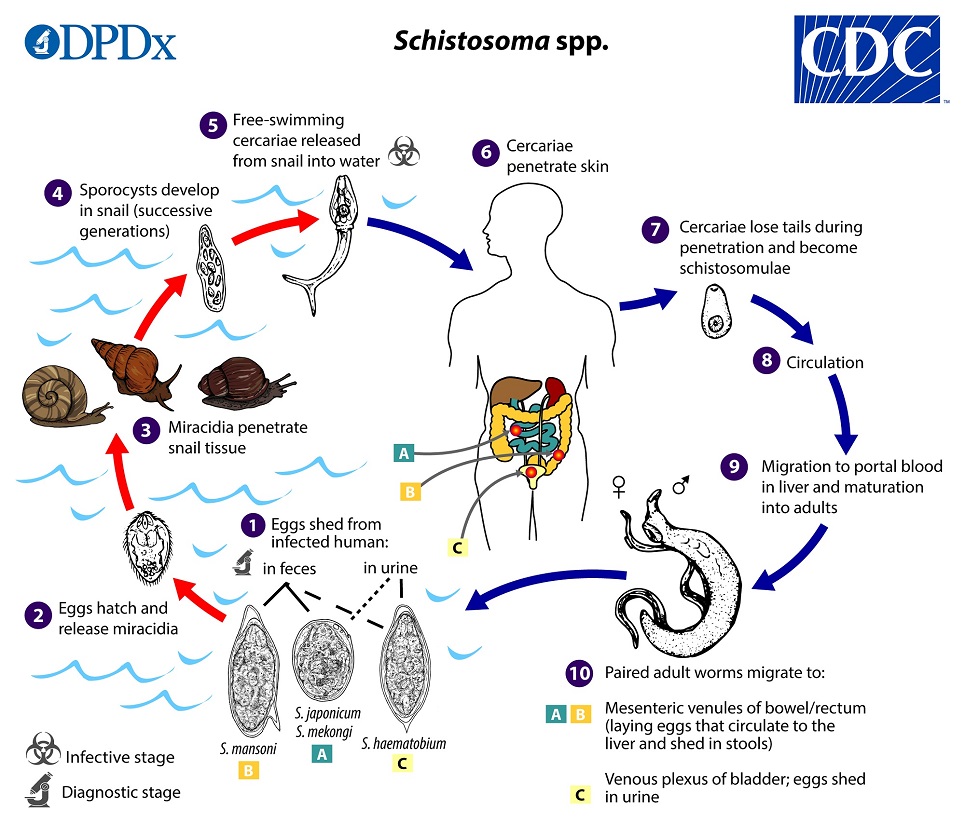
“There are multiple human-infective schistosome species, each of which infects a specific snail species found in the rivers and lakes of Sub-Saharan Africa, South-East Asia and South America. People living in areas of these regions with poor sanitation systems are constantly at risk of schistosome infection through their daily activities involving water such as swimming, washing, and agriculture,” says Lee.
The infected snails release larval offspring into the water, called cercariae, that burrow through human skin and migrate into the blood vessels by the liver where they mate and grow into mature adults. They can live for more than decade within the host and produce hundreds of eggs daily that are trapped in the body and cause organ damage. Some of the eggs released via human waste hatch in water to repeat their lifecycle.
Using a mouse model, Lee and his fellow researchers looked at stem cells from Schistosoma mansoni to discover that the larvae develop oesophageal glands before they start feeding on blood. They found that schistosomes that did not have the gland were killed by the immune cells of the mouse host.
“We believe that our research might be relevant to many parasitic worms that feed on blood, including hookworms that cause soil-transmitted helminthiasis and filarial worms that cause lymphatic filariasis,” Lee says. “Since these parasites feed on large quantities of blood, they may be equipped with an organ that plays a similar function as the oesophageal gland of S. mansoni that destroys ingested immune cells.”
“We believe that our research might be relevant to many parasitic worms that feed on blood, including hookworms that cause soil-transmitted helminthiasis and filarial worms that cause lymphatic filariasis”
Jayhun Lee, Morgridge Institute for Research
Currently, a single drug, praziquantel, is used to cure schistosomiasis, Lee says. “It is effective in killing mature schistosomes, but less so towards immature schistosomes that might be growing inside a patient. Praziquantel does not prevent re-infection. People living in endemic areas, therefore, may need to take praziquantel repeatedly. There are also reports of schistosomes that display resistance to praziquantel treatment, indicating the urgent need for new drugs.”
Stephen Davies, professor at the department of preventive medicine and biometrics, F. Edward Hébert School of Medicine Uniformed Services University of the Health Sciences, Maryland, says that “the work reveals new details of the intimate relationship that exists between schistosome parasites and their hosts, and eloquently makes the case that understanding this interaction in molecular detail will undoubtedly lead to novel treatments”.“In their work, Lee and his colleagues make two striking and unexpected discoveries,” says Davies. “First, the parasite’s oesophageal gland appears to act as a filter to the gut and fulfils a role that is critical for parasite development and survival. This is a remarkable insight into the basic biology of schistosomes that comes as quite a surprise.”
Secondly, the schistosomes seem to be vulnerable to immunological attack from host immune cells which enter the parasite gut when the organism feeds, he says. “Most previous work assumed that, if effective at all, immune cells would mount an attack on the parasite’s exterior surface. These findings pen up a new dimension to how schistosomes interact with the host immune system.”
Davies believes that the findings are applicable only to schistosomes which are unique among parasitic worms in that they spend most of their lives in the host’s bloodstream. “It makes you wonder though, whether other worms that feed on human blood, like hookworms, also employ similar strategies for protection against immune attack.”
*The photo of this article was replaced on 17 November 2022.
This piece was produced by SciDev.Net’s Asia & Pacific desk.