Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
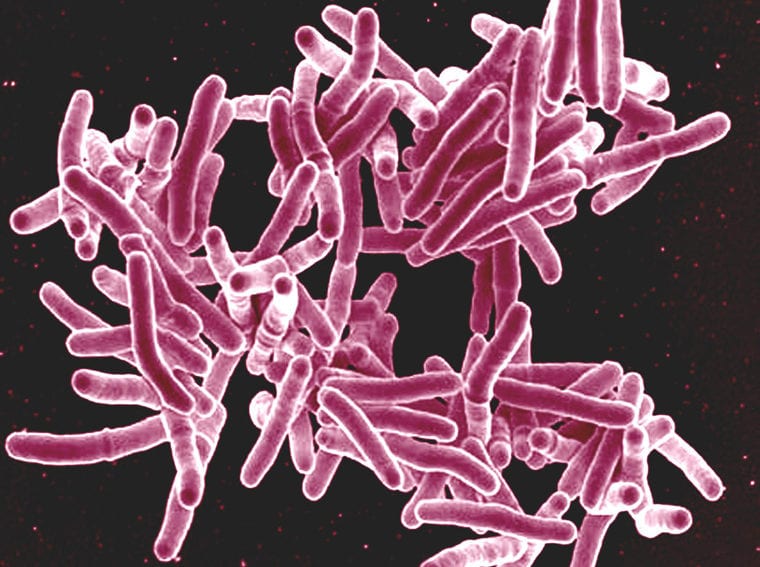
[NAIROBI] A new test developed by researchers to detect childhood tuberculosis (TB) using analysis of genes could offer hope for earlier and more accurate diagnosis of the debilitating disease.
The researchers from Kenya, Malawi, South Africa and United Kingdom who conducted the new study say the project resulted from the need to find an alternative diagnostic tool for TB in children given that those currently available have challenges.
The current diagnoses include using the skin and sputum to identify the microbe that causes TB, Mycobacterium tuberculosis, but they often lead to negative results, especially in malnourished children and those with human immunodeficiency syndrome, according to the study published in the New England Journal of Medicine last month (30 April).
“Unlike diagnosis in adults, obtaining sputum in children is usually difficult and sometimes TB in children goes unnoticed until it is fully developed.”
Andrew Brent, London School of Hygiene and Tropical Medicine, United Kingdom
Andrew Brent, a co-author and researcher with the UK-based London School of Hygiene and Tropical Medicine, adds: “Unlike diagnosis in adults, obtaining sputum in children is usually difficult and sometimes TB in children goes unnoticed until it is fully developed”.
To test whether analysis of genes could lead to better results, the researchers selected a cohort of 2,955 children suspected of having TB from Kenya, Malawi and South Africa between 17 February 2008 and 27 January 2011.
The researchers identified genes that gave clues to the presence or absence of TB from the patients’ blood samples.
According to the study, funded by the European Union and the Wellcome Trust,the researchers identified 51 genes that could distinguish between the 114 South Africa and Malawian children with TB from the 175 that had other diseases.
When the genes were used to construct a score of TB risk, the researchers were able to use it to accurately diagnose 82.9 per cent of Kenyan children with TB and correctly identify 83.6 per cent of children without the disease.
“The score may be more useful for ruling out tuberculosis than for confirming the diagnosis,” the researchers note in the journal, citing the higher proportion of patients without TB that it identified than those with the disease.
Silas Lagat, a TB specialist at the Kapsabet District Hospital in Nandi County, Kenya, says: “This test will help in reducing cases of TB among children and also will inform doctors if an individual is resistant to TB”.
Lagat believes that using genome-wide analysis could go a long way in improving TB diagnosis.
The new TB diagnostic technique has not yet been developed to become a clinical bedside test, but the researchers say they have filed patent application for it.
Link to full study in New England Journal of Medicine
This article has been produced by SciDev.Net's Sub-Saharan Africa desk.
References
New England Journal of Medicine doi 10.1056/NEJMoa1303657 (2014)