By: Pauline Okoth
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
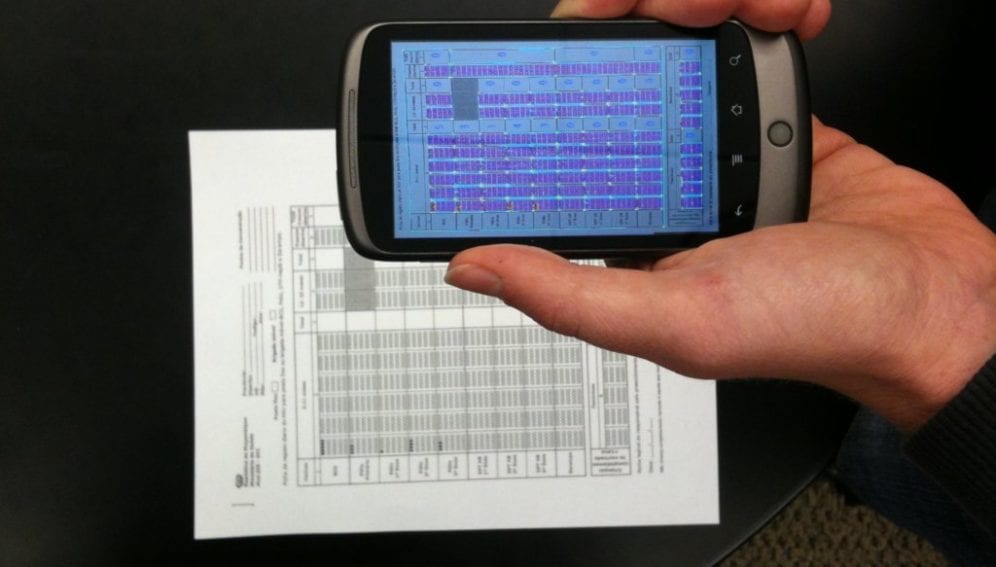
[KAMPALA] A health informatics specialist in Rwanda has developed a computer-based application to help clinicians reduce medical errors in managing HIV treatment failure.
According to Aimable Mbituyumuremyi, the developer, the application translates bulky and time-consuming paper-based guidelines on HIV treatment into a format capable of identifying causes of HIV treatment failure, contributory risk factors and making recommendations on case management.
“Most clinicians at health facilities may think that the best option is to switch the patient to a stronger combination, [but] the better option would be to correct risk factors.”
Aimable Mbituyumuremyi, Rwanda Biomedical Center
The innovation, called HIV SMART Project, was unveiled during the 5th Annual East African Health and Scientific Conference in Kampala, Uganda, last month (25-27 March).
Mbituyumuremyi says the product took 12 months to develop, with support from information and communication specialists and clinicians in Rwanda.
Antiretroviral therapy (ART) is meant to suppress HIV multiplication in patients.
Mbituyumuremyi notes that in Rwanda, clinicians face challenges in managing transition to a new treatment if HIV is not suppressed, leading to delayed or unnecessary switching between alternative treatments, which could cause drug resistance in patients.
“Most clinicians at health facilities may think that the best option is to switch the patient to a stronger combination, [but] the better option would be to correct risk factors like poor adherence… not switching to a higher level,” explains Mbituyumuremyi, a director at the Rwanda Biomedical Center.
The tool has been used to translate the Rwanda’s 2013 National guidelines for prevention and management of HIV, STIs and other blood borne infections with a specific focus on one element — supporting HIV treatment failure management.
According to Mbituyumuremyi, the application allows a clinician to systematically enter patient information, leading to a more accurate conclusion. “When using this system, it is impossible to skip even a single step in the treatment failure management decision-making process,” he says, noting that it could be used on smartphones. “It additionally prompts users to confirm previously entered information before moving to the next stage.”
The developer is hopeful that similar guidelines from other East African countries can also be built into the application to aid HIV treatment failure management.
But Shaban Mugerwa, the head of care and treatment at Uganda AIDS Control Programme, says that an accreditation criteria exist in health facilities in Uganda to provide ART, making it mandatory for such facilities to have at least a nurse, a counsellor and a prescriber.
“This team of three meet to decide when to change treatment options for HIV patients. It’s not a one-man decision. This reduces the cases of medical errors,” Mugerwa emphasised, without ruling out the possibility of human errors in HIV treatment failure management.
Some experts were concerned that health care providers could use the application to substitute their skills and knowledge, but Mbituyumuremyi noted that the application is a clinical decision support tool — and not to replace — the clinicians’ skills.
The HIV SMART Project is set for its first national field trials in Rwanda later in 2015, according to Mbituyumuremyi, adding that he hopes to develop additional modules of the application to support the management of HIV treatment side effects.
This article has been produced by SciDev.Net's Sub-Saharan Africa desk.