By: Stefano Bertozzi
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
By measuring the right things, health providers can improve HIV response and save lives, says Stefano Bertozzi of the Gates Foundation.
In his latest annual letter, Bill Gates argued that it is essential to carefully measure progress in innovation and global health. [1]
The premise makes perfect sense: what you measure and incentivise drives behaviour. This approach has transformed the landscape of health and welfare systems around the world, sometimes for good and sometimes for ill — often both.
SPEED READ
- Eight million people are being treated for HIV in developing nations but too many are dying
- Metrics such as how many start treatment fall short
- Basing evaluations on how many people stay in care will save lives
Globally, the Millennium Development Goals have provided ambitious but specific and measurable goals that countries have worked towards. At a country level, Rwanda piloted a performance-incentive approach for therapeutic, maternal and child health, and HIV/AIDS services called approche contractuelle. Both programmes have been successful and leaders are looking for ways to replicate them.
But it is also clear that measuring and incentivising the right things is not always easy.
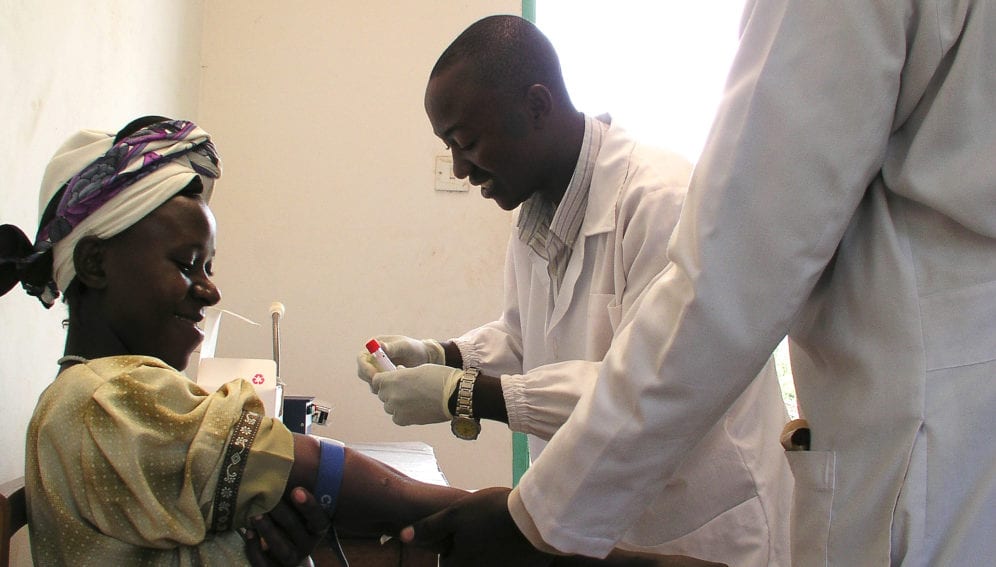
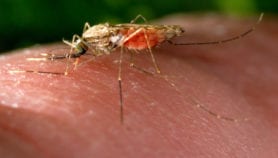
For the past ten years, the global AIDS response has been focused on expanding the coverage of prevention and treatment services. Health providers have counted how many HIV tests they administered, how many people started treatment and how many condoms were distributed.
With a lot of effort and resources, we saw these metrics rise dramatically, particularly over the past decade. Unfortunately, the metrics that ultimately matter most — the number of people contracting HIV and the number of people dying from AIDS — have not exhibited such historic improvements.
This is because while measuring the quantity of interventions is important, we also need to determine which interventions — and which approaches to them — create the greatest long-term impact.
Testing incentives
HIV testing centres in many countries, for example, often receive funding based on the number of tests they administer each year. At first glance, this approach would seem to provide the correct incentives. The more tests, the more people who know their status, right?
But this scenario ignores the fact that some individuals are at greater risk of testing positive than others, even in countries in which the epidemic is widespread across the population. For example, one centre could be deemed as highly performing for administering many tests despite it achieving this simply by frequently retesting members of the same low-risk population.
Conversely, a testing service that reaches individuals who are most likely to have become infected since their last test may find a greater number of new infections — even if fewer people are tested.
Which testing centre is doing more to contain the epidemic? Studies have shown that HIV testing and counselling have limited impact on uninfected individuals. Measuring health services by how well they target those most at risk is more efficient and effective — both in getting people on early treatment and reducing HIV transmission.
Testing and connecting
It is also important to note that simply notifying patients of their status has not been shown to have much impact. Instead of HIV 'testing and counselling', we must incentivise HIV 'testing and connecting'.
For those who test positive, this means immediately connecting them to care. For those who test negative, it means connecting them to appropriate prevention services. Without these connections, the benefits of testing cannot be realised.
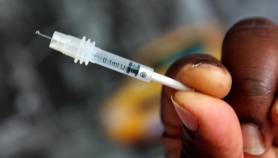
Similarly, global targets and national goals have focused on increasing the number of HIV-positive individuals on treatment. At the 2012 International AIDS Conference, UNAIDS (the Joint UN Programme on HIV/AIDS) reported the tremendous news that the number of these individuals on treatment in the developing world had surpassed eight million in 2011 and repeated its call to reach the remaining seven million people eligible for treatment but who still do not have access.
However, antiretroviral treatment only prevents illness and death when patients receive the right drugs and adhere to their prescribed regimens. This has proven to be a difficult goal in many places. Some treatment centres have dropout rates of more than a third of their patients per year, and other centres fail to successfully control HIV in many of their patients.
The hard truth is that fewer lives are being saved than would be expected with eight million people on treatment.
Tracking patients' health
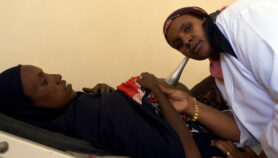
So what should we do? Instead of just counting the numbers of individuals beginning treatment, we need to evaluate treatment centres by how many people are successfully retained in care and consistently take their medications. An even stronger approach would be to monitor whether HIV replication is suppressed in each patient.
These are difficult tasks, but they are achievable. Clinics can measure and report how many of their patients stay alive, and determine why some clients stop coming for care and can no longer be reached. Reductions in the price of viral load tests can help more clinics track patients' health and provide clinicians with valuable information on how to best proceed with treatment.
As new performance measures are introduced, it is critical to understand which ones provide the best return on investment — that is, yield the greatest gains in health at the lowest cost. This is a new area of focus that has been recognised by others, including the US Institute of Medicine in its recent evaluation of the President's Emergency Plan for AIDS Relief (PEPFAR). [2]
By measuring the right things, we can better gauge the effectiveness of our HIV response, drive better performance and ultimately save more lives.
Stefano Bertozzi is director of HIV for the Bill & Melinda Gates Foundation, headquartered in Seattle, United States.
References
[1] Gates, B. Annual letter (Bill & Melinda Gates Foundation, January 2013)
[2] Institute of Medicine Evaluation of PEPFAR (The National Academies Press, 2013)