By: Richa Malhotra
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
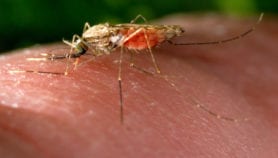
A low-cost, portable device that can detect malaria in people who show no symptoms is soon to be tested in Africa.
This ‘mobile bio-lab’, under development by Dutch company Amplino, aims to help health workers identify asymptomatic malaria sufferers using a sensitive molecular technique.
“Current malaria tests used in the field are not very sensitive and do not detect a small amount of malaria infection. If you want to eliminate malaria you have to make sure that people you are testing do not have any parasite left in the body.”
Erwan Piriou, Médecins Sans Frontières
People who show no symptoms, but are nonetheless infected with malaria, can frustrate prevention efforts by unknowingly infecting parasite-free mosquitos.
While malaria tests are already in widespread use in Africa, most are ‘dipstick’ rapid diagnostic tests (RDTs) that detect proteins from the parasite but do not give a precise measure of their concentration in the blood.
As asymptomatic carriers have low concentrations of the malaria-causing Plasmodium parasite in their blood, these tests are often not sensitive enough to detect the signature proteins.
But the new test is different. According to the developers it uses qPCR (quantitative polymerase chain reaction), a much more sensitive biochemical process that takes the tiny amounts of parasite DNA in carriers’ blood and amplifies it so it can be detected. Fluorescent dye that binds to the DNA then indicates infection.
qPCR is usually a costly technique and difficult to do outside of a lab because of the need to extract DNA. Amplino has simplified the process by taking blood from a finger prick and dabbing it on a cartridge that is inserted into the device, which then carries out qPCR — at a fraction of the cost of a full-size lab.
The qPCR protocol for detecting Plasmodium DNA from a blood sample was developed at the Royal Tropical Institute in Amsterdam. [1]
While the test can identify if the sample is infected with Plasmodium, it cannot differentiate between different species of the parasite.
Amplino’s developers are hoping the device will help health workers identify malaria carriers who are not currently detected. Wouter Bruins, one of Amplino’s founders, says: “We are not aiming at 90 per cent of malaria patients. They are doing fine with rapid diagnostic tests.”
The test may be especially important for asymptomatic pregnant women, who can develop complications if their infection remains undetected. The parasite can hide in the placenta where it is hard to detect, the company notes.
According to Amplino, the device could cost as little as US$250, much less than typical qPCR equipment, which costs ten times as much and also needs a lab and technicians
Mapping incidence
The device will also be equipped with GPS (Global Positioning System) and a mobile data connection to send the test results to Amplino’s database, which the company hopes will help map the incidence of malaria.
“Those who provide malaria diagnostics to doctors and healthcare workers do not get any feedback on how much these are used,” says Jelmer Cnossen, co-founder of Amplino and a researcher at Delft University of Technology in the Netherlands.
“There is a big gap between the supply of these devices and the results from them.”
Amplino plans to test data connectivity in Malawi and Zambia in December, and will also test blood samples with local research groups such as the Johns Hopkins Malaria Research Institute at Macha, Zambia.
Following lab trials of the prototype Amplino aims to take the device into field trials next year, where it will test the device with patients.
Erwan Piriou, a public health researcher and laboratory advisor at Médecins Sans Frontières, Amsterdam, says: “I see some great uses for such tools. One is not necessarily in high-malaria burden countries but where authorities are working towards the elimination of malaria.
“Current malaria tests used in the field are not very sensitive and do not detect a small amount of malaria infection. If you want to eliminate malaria you have to make sure that people you are testing do not have any parasite left in the body.”
References
[1] Journal of Clinical Microbiology doi:10.1128/JCM.01426-12 (2012)