By: Hannah Kuper
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
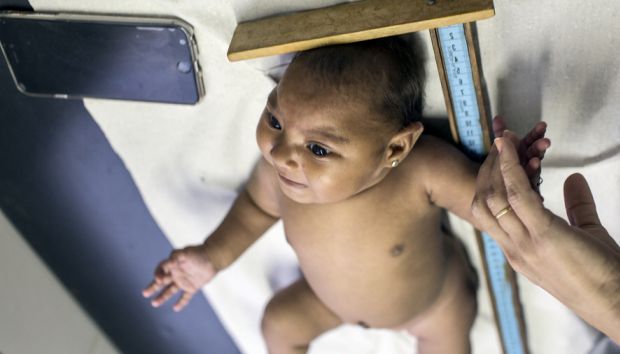
About 4,000 babies have now been born with microcephaly — abnormally small heads, often with underdeveloped brains — in Brazil alone. Evidence is mounting that this is because of infection during pregnancy by the mosquito-borne Zika virus. Media attention on the epidemic has mainly focused on how to stop babies being born with microcephaly, whether by killing mosquitoes, finding a vaccine or easing abortion laws. Similarly, the WHO strategic response to Zika focuses on preventing outbreaks and controlling them when they occur. [1]
But what are the implications for the thousands of babies born with microcephaly? This is barely considered within the WHO response: disability is mentioned just twice.
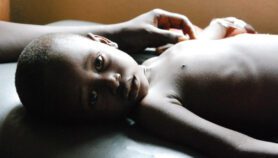
Microcephaly has many different causes, all with varying impacts. This means the implications for babies with what appears to be Zika-related microcephaly are not yet clear. But we do know that microcephaly can cause wide-ranging physical and mental disabilities, including learning difficulties, hearing problems and physical impairments. There is already evidence from Brazil that Zika-related microcephaly is linked to eye disease. [2]
“Interventions are therefore needed to teach parents to better stimulate their child or pick up on cues from their children about what they need.”
Hannah Kuper
So the support babies need will vary. But some basic steps will benefit all of them. Firstly, intervening within the first year of life will improve things for babies at risk of disabilities. [3] Programmes should ideally target both the baby’s motor and cognitive skills, as these are intertwined and reinforce each other: interventions such as physiotherapy or playing games will stimulate the child’s overall development.
These programmes should take place within the community, rather than at central clinics, to minimise dropout rates. Information and communications technologies can help too: one programme in India for children with disabilities uses community workers and mobile tech to deliver interventions — how to best feed the child, for example — informed by evidence.
Despite Brazil’s strong primary healthcare service, support services for children with disabilities are limited. Philanthropic national organisations, such as APAE, fill some of the gaps. But essentially it will be parents, in particular mothers, will be mainly responsible for caring for children with microcephaly. Interventions are therefore needed to teach parents to better stimulate their child or pick up on cues from their children about what they need.
The parents of these babies will also need emotional support, particularly as a lot of stigma and discrimination is reported around childhood disability in Brazil. Evidence shows that parents of children with disabilities can suffer acute anxiety and may feel socially isolated. [4] Parents may also face financial pressures as they forego work to look after their child or pay for extra healthcare.
Establishing support groups for parents will help provide emotional and practical support. [4] Such groups have been set up around the world for the parents of children with cerebral palsy, providing a forum for parents to come together and learn skills but also share experiences. Schemes like these could work in Brazil.
Governments and international health campaigners must act now to ensure these kids aren’t forgotten, so they and their families can have the best lives possible.
Hannah Kuper is codirector of the International Centre for Evidence in Disability at the London School of Hygiene & Tropical Medicine, United Kingdom. The centre is on Twitter as @ICED_LSHTM, and Kuper can be contacted on [email protected]
References
[1] Zika strategic response framework & joint operations plan (WHO, February 2016)
[2] Bruno de Paula Freitas and others Ocular findings in infants with microcephaly associated with presumed Zika virus congenital infection in Salvador, Brazil (JAMA Ophthalmology, 9 February 2016)
[3] Alicia Spittle and others Early developmental intervention programmes provided post hospital discharge to prevent motor and cognitive impairment in preterm infants (Cochrane Database of Systematic Reviews 2015, 24 November 2015)
[4] Sarah Nakamanya and others Maternal experiences of caring for an infant with neurological impairment after neonatal encephalopathy in Uganda: a qualitative study (Disability and Rehabilitation, 17 October 2014)
[5] UN convention on the rights of persons with disabilities (UN, 2006)