By: Claudia Caruana
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
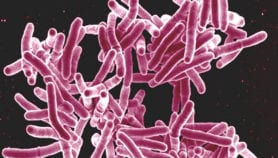
[NEW YORK] Although malaria and tuberculosis are very different diseases — malaria is caused by a parasite while tuberculosis by a bacterium — their treatments might one day both include the use of artemisinin.
In a promising pre-clinical study published last month (December), Robert Abramovitch, a Michigan State University microbiologist and TB researcher and his colleagues, have shown how this ancient herb might be useful in curbing TB as well.
Abramovitch says as part of their disease cycles, both malaria and TB depend on a molecule called heme.
“Although, this is an early lab study, this finding is important because it is a new way to kill the TB bacterium.”
Robert Abramovitch, Michigan State University
Already, artemisinin, a Chinese herb isolated from the plant artemisinin annua, is being used as a first-line treatment for malaria. It works by killing and reducing the number of plasmodium parasites in human blood.
But now, it might have a new role.
In the study, artemisinin stopped the ability of TB-causing bacteria to become dormant, a key problem in treating the disease.
The dormancy of TB often makes the use of antibiotics ineffective and lengthens treatment. TB can remain dormant and symptomless in the body for many years and then become re-activated.
TB bacterium, Abramovitch points out, need oxygen to thrive in the body, but the immune system starves it to control the infection. Because artemisinin is attracted to heme, which acts as an oxygen sensor, the disease does not go dormant. This is important for continued treatment.
According to the Centres for Disease Control and Prevention in the US one third of the world’s population is infected with TB, and the disease killed 1.8 million people in 2015.
Abramovitch’s group screened more than 540,000 possible compounds in the study to find a new pathway to prevent the TB bacterium from going into dormancy. Artemisinin and several other compounds were found to stop the bacteria from going dormant.
“Although, this is an early lab study, this finding is important because it is a new way to kill the TB bacterium,” he says.
However, Abramovitch stresses that it “would be premature” to use artemisinin as a TB treatment now, even though this is an “encouraging study.”
“Substantial additional work needs to be undertaken to determine the interactions and safety with standard TB therapy drugs such as isoniazid, rifampicin, pyrazinamide, and ethambutol. We envisage using a dormancy inhibitor — one possible one being artemisinin — as an adjunct to standard TB therapy,” he says.Abramovitch says it could be several years, “before artemisinin and the new class of inhibitors will be ready for the clinic,” but the study could be an important starting point.
Martin Voskuil, professor of immunology and microbiology at the University of Colorado, Denver, says: “The discovery of a compound that kills M. tuberculosis opens the door to treatment strategies that may significantly shorten therapy of both drug sensitive and drug resistant infections."
This piece was produced by SciDev.Net’s South-East Asia & Pacific desk.
References
Huiqing Zheng, Christopher J Colvin, Benjamin K Johnson, Paul D Kirchhoff, Michael Wilson, Katriana Jorgensen-Muga, Scott D Larsen, Robert B Abramovitch. Inhibitors of Mycobacterium tuberculosis DosRST signaling and persistence. Nature Chemical Biology, 2016; DOI: 10.1038/nchembio.2259