By: Saleem Shaikh
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
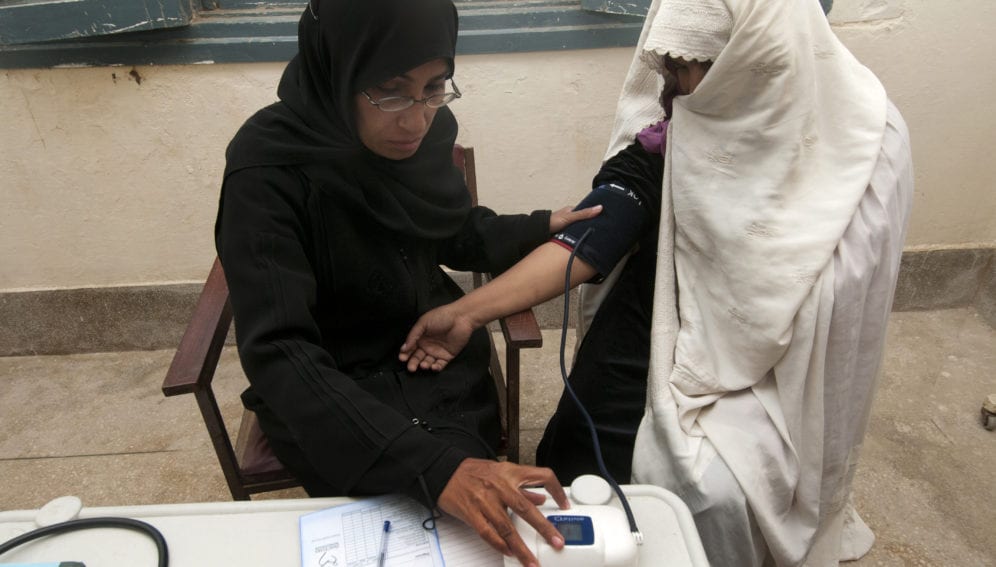
[ISLAMABAD] Pakistan is eyeing doorstep healthcare to female HIV patients in the deeply conservative Khyber Pakhtunkhwa province where women are not allowed outdoors unless accompanied by closely-related male family members.
“For such health services, female health workers, who already provide at-home maternity and vaccination services across Pakistan, could be engaged,” saysBaseer Khan Achakzai, national manager of the AIDS programme at the federal ministry of health services.
“Changing society’s perceptions and attitudes to favour women’s healthcare, and autonomy to seek healthcare and make economic decisions, are important to improving women’s access to medical treatment.”
Abubakar Saeed, COMSATS Institute of Information Technology
Achakzai tells SciDev.Net that plans to provide anti-retroviral therapy (ART) to female sufferers at their homes are already under discussion with higher government authorities. He says this would ”significantly help cope with outside mobility constraints” on them.
A study, published in the July-August issue of Journal of the Association of Nurses in AIDS Care found that restrictions on women’s mobility, under the religiously-motivated parda (seclusion) system, are particularly severe in the Khyber Pakhtunkhwa that adjoins Afghanistan.
Often husbands, brothers or other closely-related male family members show lack of support or are unavailable for clinical appointments and medical care, says the study which involved interviews with 21 women living with HIV.
If they are living with in-laws, the problem becomes graver since they are required to justify absences from home. This can be cumbersome if the patient wishes to conceal her HIV status to avoid social stigma.
Factors inhibiting women’s access to ART and other healthcare services include distance to the HIV clinic and ages of their children, according to the study.
“The restrictions are more in the conservative Khyber Pakhtunkhwa than in the country’s three other provinces,” Abubakar Saeed, lead author of the study and scientist at the Islamabad-based COMSATS Institute of Information Technology, tells SciDev.Net.
Saeed says that many women learn of their HIV-positive status only after undergoing medical tests recommended to them for some other health issues.
The study suggests that policy-makers understand the nuances of local cultures in which women seek HIV treatment so that practical, culturally appropriate and acceptable programmes can be devised.“Changing society’s perceptions and attitudes to favour women’s healthcare, and autonomy to seek healthcare and make economic decisions, are important to improving women’s access to medical treatment,” says Saeed, adding that faith leaders, teachers, health workers and media practitioners play roles in positively transforming perceptions and attitudes.
This piece was produced by SciDev.Net’s Asia & Pacific desk.