By: Fatima Arkin
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[MANILA] A coalition of health experts is pressing governments in the Asia-Pacific to endorse the global strategy of the WHO to fight viral hepatitis to reduce its threat.
The disease is endemic in the region but awareness is low, and only less than one per cent of people who need treatment receive it, according to the Singapore-based nonprofit Coalition to Eradicate Viral Hepatitis in Asia Pacific (CEVHAP) which organised a symposium on 24 February in Tokyo, Japan.
In the Asia-Pacific alone, one million people die from viral hepatitis each year, three times the mortality rate of HIV/AIDS. In 2015, there were 6 to 10 million new cases of chronic hepatitis, says CEVHAP.
Chronic hepatitis B is most prevalent among the general adult population aged over 25 because they were born before the introduction of the hepatitis B vaccine to national immunisation programmes.
“If the 2030 global hepatitis targets proposed by the WHO are achieved, it is possible to eliminate hepatitis by 2030.”
By Stephen Locarnini, co-chair of CEVHAP
The proposed WHO strategy will come to a vote in May at the World Health Assembly in Geneva, the WHO’s decision-making body which is attended by delegations from all WHO member states.
The strategy offers a set of priority actions for governments and the WHO to stop hepatitis transmission and increase accessible care. One notable target is for governments to achieve 90 per cent diagnosis by 2030, up from the current level of less than five per cent.
While viral hepatitis has featured high on the agenda at many of the WHO’s annual regional meetings since the inaugural World Hepatitis Summit held in September 2015 in Glasgow, Scotland, its prioritisation has been mixed.
Last October in Guam, the WHO Western Pacific committee approved a regional action plan to fight hepatitis and has started to implement it in high-burden countries such as Vietnam. This plan is aligned with the WHO’s proposed global strategy.
But hepatitis failed to make it on the agenda of the WHO’s South-East Asia regional committee meeting in September 2015 in Timor-Leste.
“If the 2030 global hepatitis targets proposed by the WHO are achieved, it is possible to eliminate hepatitis by 2030,” Stephen Locarnini, co-chair of CEVHAP and head of research and development at the Victorian Infectious Diseases Reference Laboratory in Australia, tells SciDev.Net. “Failure to keep to the targets proposed by the draft strategy will result in a significant setback.”
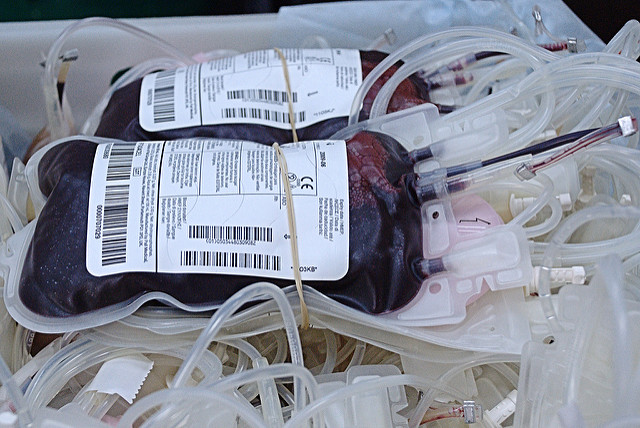
Locarnini says people of all ages, ethnic groups and genders can be at risk of hepatitis C when receiving unsafe healthcare services, such as contaminated blood transfusion. Low-income populations and indigenous people are particularly vulnerable as they are more likely to be exposed to unsafe practices.
Kenji Shibuya, a global health professor at the University of Tokyo, tells SciDev.Net that to get more attention on hepatitis, it would be useful to link with and learn from experts involved in fighting other diseases, particularly HIV/AIDS.
“They did very well and were very successful in putting that agenda into health system development and financing,” Shibuya notes.
This piece was produced by SciDev.Net’s South-East Asia & Pacific desk.