By: Yao-Hua Law
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[KUALA LUMPUR] From South Asia to the Pacific islands, more than 220 million people are diabetic, making up almost 55 per cent of the world total. Half of these diabetes cases are undiagnosed, which may later cause life-threatening complications.
Earlier and wider detection of diabetes can be achieved if the current diagnosis method, blood glucose analysis, is complemented with haemoglobin A1C (HbA1C), says a review in the Asian Pacific Journal of Tropical Biomedicine, which was recently republished online (19 March) and now freely accessible unlike the early limited access.
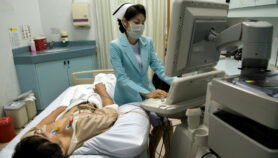
Prior to 2010, measuring blood glucose was the gold standard to diagnose diabetes, using either a fasting plasma glucose test (FPG) or oral glucose tolerance test. Both tests require patients to fast, which is inconvenient for those who have to travel far to a clinic. Also, FPG results can vary more than 12 per cent between tests.
“The results of a FPG depend on how well you fast and what you ate the night before. It is confusing to diagnose someone diabetic in one test but the next test shows normal results,” says Usman Malabu, an endocrinologist and associate professor of medicine at James Cook University in Queensland, Australia, and senior author of the study.
Looking for a more reliable alternative to blood glucose analysis, doctors turned to HbA1C. In blood cells, HbA1C forms when glucose binds to haemoglobin. The more glucose there is in the blood and the older the cell, the more HbA1C there is. HbA1C levels can indicate blood glucose levels over the past three months.
Since the 1980s, doctors have been using HbA1C to measure and monitor blood glucose levels in diabetic patients. Fasting is not required and results are available within minutes. The test also produces consistent results with less than one per cent variation.
In 2010, the American Diabetes Association (ADA) recommended HbA1C as a diabetes diagnostic tool in its clinical practice recommendations. Europe followed suit. In the Asia-Pacific, New Zealand has already adopted HbA1C.
By late 2015, Malaysia too will adopt HbA1C as a diabetes diagnostic tool in its new revision of clinical practice guidelines, Nor Azmi Kamaruddin, president of the Malaysian Endocrine and Metabolic Society, tells SciDev.Net.
A recent national health survey allowed Malaysian physicians to establish HbA1C standards in diabetes diagnosis. Malaysia will use a HbA1C cut-off point of 6.3 per cent, slightly lower than the ADA’s recommended 6.5 per cent.
Kamaruddin expects neighbouring South-East Asian countries to soon adopt HbA1C. Some countries though may lag “because of inadequate healthcare financing,” she says.
The higher cost of HbA1C is offset by its convenience and reliability. “HbA1C will help us diagnose more patients, reduce the number of undiagnosed diabetes and manage diabetic patients earlier,” says Kamaruddin. “If we don’t use HbA1C, we miss picking up to 20-25 per cent of diabetic individuals.”
Countries that will adopt HbA1C should “prepare for an immediate hike in diabetes prevalence, which is good,” says Malabu explaining that early diagnosis and management saves on the cost of diabetes complications in later years, such as renal dialysis and prolonged hospitalisation from non-healing foot ulcers.
“HbA1C will revolutionise the way we see diabetes,” says Malabu. “It will show the true picture of the diabetes epidemic.”
>Link to abstract in Asian Pacific Journal of Tropical Biomedicine
This article has been produced by SciDev.Net's South-East Asia & Pacific desk.
References
Asian Pacific Journal of Tropical Biomedicine doi: 10.1016/S2221-1691(14)60214-8 (2014)